Worm That Temporarily Disables Pain Sensation: and yes, that’s exactly what’s happening in real laboratories right now. Scientists have identified how a parasitic worm can temporarily quiet the body’s pain and itch signals, allowing it to enter through the skin almost unnoticed. That discovery isn’t just biologically fascinating — it could eventually reshape how we treat chronic pain in the United States and around the world. Let’s talk about this in a way that makes sense whether you’re ten years old or a practicing physician. Pain is your body’s built-in warning system. It’s like a smoke alarm in your house. When something harmful happens, your nerves send signals to your brain that say, “Hey! Pay attention!” But this worm has figured out a way to sneak past that alarm system. And researchers believe understanding that trick could open doors to safer, non-addictive pain treatments — something America urgently needs.
Table of Contents
Worm That Temporarily Disables Pain Sensation
Researchers investigating a worm that temporarily disables pain sensation are uncovering one of the more fascinating intersections of infectious disease and neuroscience. By studying how Schistosoma mansoni suppresses TRPV1 neurons, scientists are gaining insights that could influence the future of pain management in America. While still in early stages, this research highlights how evolutionary biology can guide innovation. In a nation grappling with chronic pain and opioid dependency, discoveries like this offer cautious but meaningful hope.
| Topic | Details |
|---|---|
| Worm Studied | Schistosoma mansoni |
| Disease Caused | Schistosomiasis |
| People Affected Globally | ~240 million (WHO) |
| U.S. Chronic Pain Cases | ~50 million adults (CDC) |
| Neurons Targeted | TRPV1+ sensory neurons |
| Research Journal | The Journal of Immunology |
| Drug Approval Oversight | U.S. FDA |
| Official Health Resource | https://www.who.int/news-room/fact-sheets/detail/schistosomiasis |
Understanding the Worm That Temporarily Disables Pain Sensation Behind the Discovery
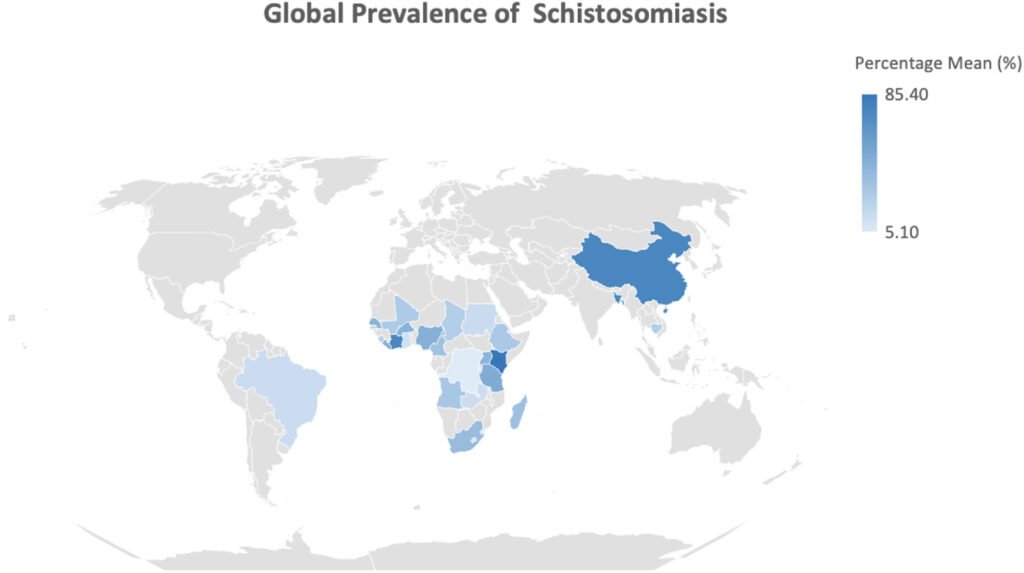
The parasite at the center of this research is Schistosoma mansoni, one of several species responsible for schistosomiasis, a tropical disease recognized by the World Health Organization (WHO). According to WHO data, approximately 240 million people worldwide require treatment for schistosomiasis every year. That’s not a small number — that’s nearly the population of Texas, Florida, and New York combined.
The parasite’s life cycle is complex. It starts in freshwater snails. The larvae, known as cercariae, are released into water and can penetrate human skin when someone swims, bathes, or wades in contaminated water. In many cases, people feel little to no pain when this happens.
That’s unusual. When bacteria or viruses enter the body, inflammation and irritation typically occur. But this worm seems to glide in quietly. Scientists wanted to know why.
The Science of Pain: Breaking It Down Simply
To understand what researchers discovered, we need to talk about nerves — specifically something called TRPV1+ sensory neurons.
Think of TRPV1 neurons as electrical wires. They carry signals from your skin to your brain. They respond to:
- Heat
- Spicy chemicals (like capsaicin in hot peppers)
- Tissue damage
- Inflammation
If you’ve ever bitten into a jalapeño and felt that burning sensation, that’s TRPV1 doing its job.
According to the National Institute of Neurological Disorders and Stroke (NINDS), pain perception begins when specialized sensory receptors detect potentially damaging stimuli.
When TRPV1 neurons activate, they don’t just send pain signals. They also help trigger immune responses. That’s key.
What researchers observed is that Schistosoma mansoni releases molecules that reduce TRPV1 neuron activity during skin penetration. In simpler terms: the worm turns down the volume on the body’s pain alarm.
Worm That Temporarily Disables Pain Sensation: What the Research Shows
Studies published in The Journal of Immunology describe how the parasite suppresses neural activation in laboratory models. Researchers observed decreased firing of TRPV1 neurons when exposed to parasite-derived molecules.
Importantly, this suppression appears temporary. The parasite doesn’t permanently damage nerves; it simply dampens their responsiveness long enough to establish infection.
For scientists, that’s a goldmine of insight.
If a naturally occurring molecule can selectively quiet pain without destroying nerve tissue, it raises a powerful question:
Could we replicate that mechanism safely in a controlled medical setting?
Why Does the Worm That Temporarily Disables Pain Sensation Matters in the United States?
Chronic pain is one of the most common medical conditions in America. The CDC estimates that over 50 million U.S. adults live with chronic pain. About 20 million experience high-impact chronic pain that limits daily activities.
Now combine that with the opioid crisis. According to the CDC, more than 80,000 opioid-related overdose deaths occurred in 2022 alone.
Doctors across America are searching for safer pain management strategies. Non-opioid alternatives are in high demand. Pharmaceutical companies are investing billions into research for targeted pain therapies that don’t carry addiction risk.
That’s where this worm research intersects with public health reality.
If scientists can isolate and synthesize the molecules responsible for suppressing TRPV1 neurons — without introducing infection — they may create a new class of pain medication.
How Researchers Are Moving Forward?
Scientific progress doesn’t happen overnight. It moves step by step.
First, researchers identify the exact compounds secreted by the parasite during skin penetration. This requires protein analysis, molecular mapping, and advanced imaging techniques.
Second, they test those compounds in controlled laboratory environments to determine whether they suppress pain signals without affecting other critical nerve functions.
Third, safety evaluation begins. A molecule that blocks pain but prevents someone from sensing dangerous heat could pose serious risks. Previous experimental TRPV1 blockers sometimes caused impaired temperature regulation, which halted their development.
That process includes:
- Preclinical research
- Phase I safety trials
- Phase II effectiveness trials
- Phase III large-scale studies
It can take 10 to 15 years from discovery to approved medication.
Professional and Career Implications
For healthcare professionals, this discovery touches multiple disciplines:
Neurologists gain new insight into sensory signaling.
Immunologists explore how nerves and immune responses interact.
Pharmacologists investigate new drug targets.
Public health experts analyze global disease patterns.
The global pain management drug market is projected to exceed $90 billion by 2030, according to industry forecasts. That represents significant economic and career opportunity.
Students entering biomedical research, neuroscience, or pharmaceutical development may find this area especially promising.
Ethical Considerations and Safety Concerns
It’s important to emphasize that Schistosoma mansoni is harmful. Schistosomiasis can cause chronic organ damage, liver complications, and long-term disability.
The goal is not to use the parasite as treatment. Instead, researchers aim to learn from its biology.
Ethical medical research requires strict safety standards. Any therapeutic application must undergo rigorous testing to ensure:
- No infection risk
- No immune suppression
- No unintended nerve damage
- No long-term toxicity
The United States operates under strong regulatory oversight through the FDA and institutional review boards to protect patient safety.
Real-World Applications Beyond Pain
Interestingly, this discovery may also impact autoimmune disease research.
Because TRPV1 neurons interact with immune cells, suppressing these pathways could theoretically reduce inflammatory disorders.
Conditions like:
- Rheumatoid arthritis
- Psoriasis
- Neuropathic pain syndromes
might one day benefit from targeted modulation of sensory nerves.
However, researchers caution that this is early-stage science. Translation from laboratory findings to clinical therapy requires years of validation.
Practical Advice for Medical Professionals
For clinicians and healthcare administrators, staying informed is critical.
Monitor peer-reviewed journals discussing TRPV1 modulation.
Attend neurology and pain management conferences.
Educate patients on evidence-based non-opioid alternatives currently available, such as physical therapy, cognitive behavioral therapy, and FDA-approved non-opioid medications.
Avoid overpromising emerging therapies until clinical trials confirm safety and effectiveness.
Pain management is evolving rapidly. Integrating biological insights responsibly is essential.
Antarctic Mission Mystery — Research Robot Vanishes During Major Expedition
Scientists Worry a New AI Tool Could Flood Research With Low-Quality Studies
Researchers Find Ancient Whale Fossils Hundreds of Kilometres Inland