In the summer of 1665, as infection spread through crowded streets and narrow alleys, residents turned to London’s 1665 Plague death lists — the Bills of Mortality — to judge whether they should stay or flee. The weekly records, compiled by parish officials, became a practical survival guide, allowing citizens to track where disease was spreading across the city.
Table of Contents
London’s 1665 Plague
| Key Fact | Detail/Statistic |
|---|---|
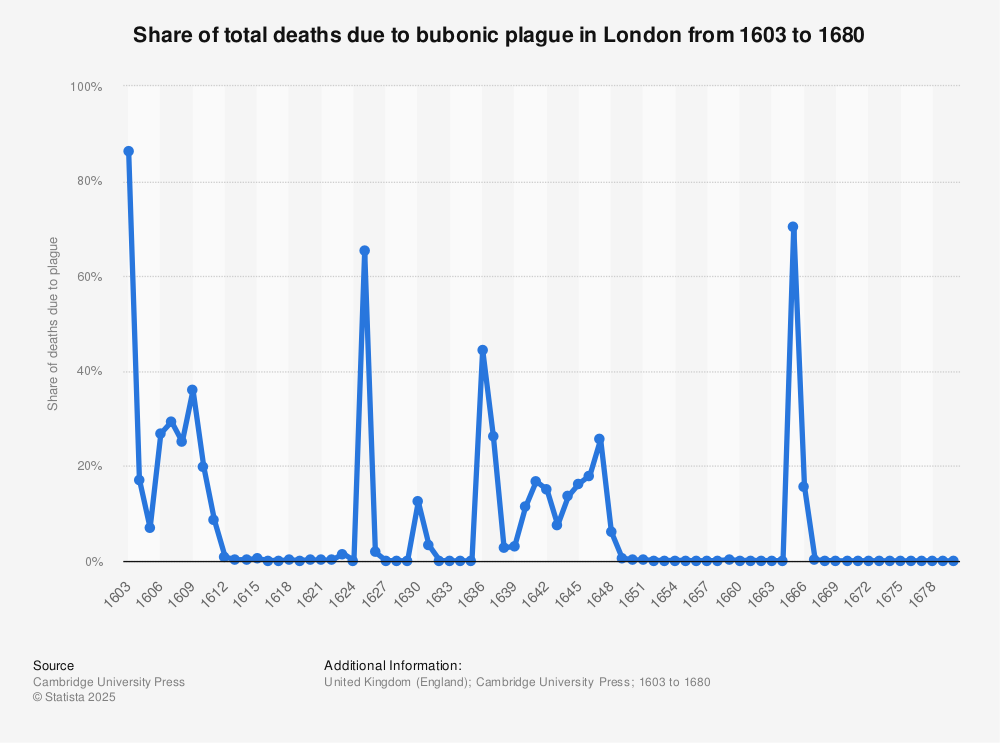
| Peak mortality | Up to 7,000 deaths per week in September 1665 |
| Estimated total deaths | 75,000–100,000 (about one-fifth of London’s population) |
| Scientific breakthrough | John Graunt analyzed mortality data in 1662 |
When the epidemic ended, London resumed ordinary life, but the weekly lists remained. The city had learned that careful record-keeping could reveal invisible threats. The principle endures: long before modern medicine, information itself became a form of protection.
What Was London’s 1665 Plague Data System?
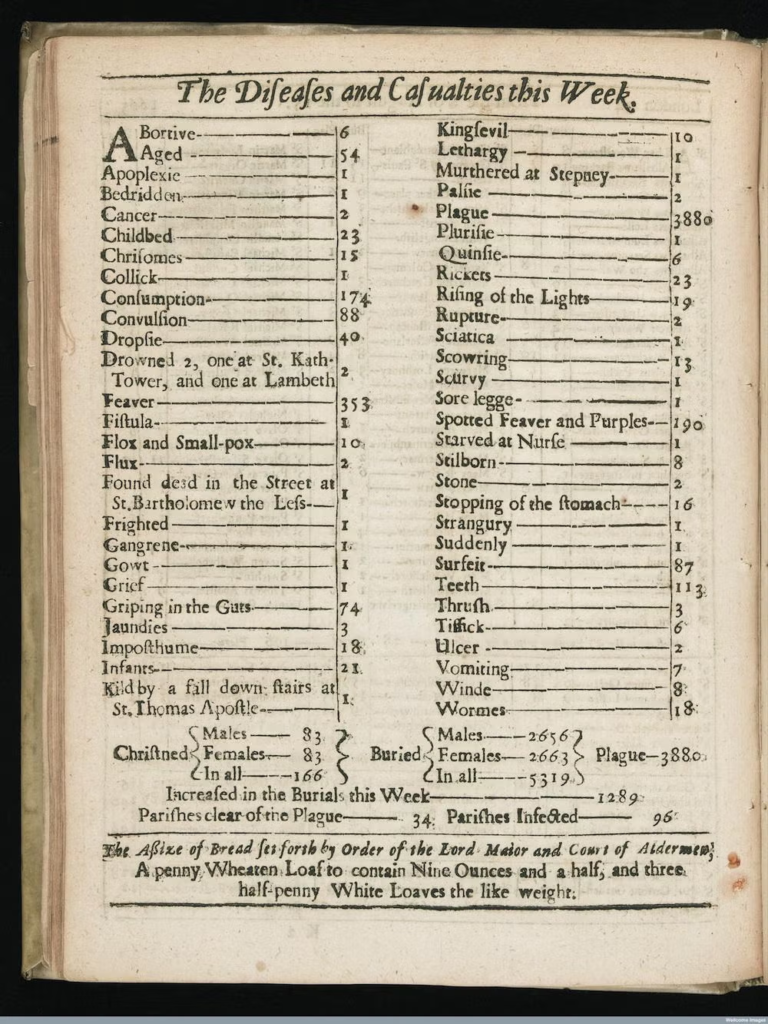
London’s 1665 Plague information system relied on weekly printed Bills of Mortality, documents listing burials by parish and suspected causes of death. The reports were posted publicly and sold on the streets, making them accessible to literate residents and merchants.
Parish clerks gathered numbers from church burial registers. Specially appointed “searchers” examined bodies and recorded symptoms such as swellings, fever, or delirium, all signs associated with plague.
The method lacked medical accuracy. Yet it created something unprecedented: a citywide health monitoring network.
Historians describe the lists as an early form of epidemic surveillance.
“People were reading statistics before statistics was a science,” wrote public-health historian Paul Slack in research on early modern England.

How Residents Used the Information
Every Thursday, Londoners awaited the latest publication. The numbers determined personal decisions.
Citizens first checked their own parish. A small rise suggested caution. A rapid jump signaled imminent danger.
Wealthier families hired coaches and left immediately. Diaries from the period describe a steady flow of wagons departing the city.
The English diarist Samuel Pepys recorded the moment in June 1665 when deaths reached alarming levels. He wrote that London had become “sad and sickly,” and noted neighbors quietly leaving overnight.
Who Could Escape — and Who Could Not
Flight became the most effective protection. But only certain groups could manage it.
Merchants relocated business temporarily. Landowners moved to country estates. Students left universities.
Poor laborers remained.
Authorities also imposed quarantine rules. When a house showed infection, officials nailed the door shut and marked it with a painted red cross and the words: “Lord have mercy upon us.”
This practice often trapped entire families inside, including healthy members.
Early Evidence of Behavioral Public Health
The death lists influenced behavior in measurable ways. Trade routes shifted. Markets closed earlier. Church attendance declined.
In modern terminology, citizens were adjusting risk based on data — a behavior similar to how people monitor infection dashboards today.
Researchers in historical epidemiology say the reaction shows people intuitively understood probability, even without scientific explanation.
The Emergence of Statistical Thinking
Before the epidemic, London merchant John Graunt had already examined mortality records. In 1662, he analyzed decades of data and identified regular patterns in births and deaths.
He calculated average life expectancy and noticed seasonal disease cycles. The work later earned recognition from the Royal Society of London, the scientific body founded in 1660.
Graunt’s study demonstrated that disease could be measured rather than interpreted as divine punishment.
Scholars now consider the analysis the foundation of demography and epidemiology.
Why the System Worked Despite Medical Misunderstanding
Seventeenth-century physicians believed plague spread through foul air, known as miasma theory. They burned incense, carried herbs, and avoided certain winds.
The real cause — bacteria carried by fleas on rats — would not be discovered until 1894 by Alexandre Yersin.
Yet the weekly death counts still provided reliable warning signals.
Because rats moved locally through dense housing, outbreaks spread neighborhood by neighborhood. A rise in burials meant infection had already begun circulating nearby.
The records therefore predicted risk days or weeks before symptoms appeared widely.
Life Inside the Infected City
Contemporary accounts describe silent streets and shuttered homes. Bells rang constantly for funerals. Night workers called “watchmen” guarded quarantined houses.
At night, carts moved through streets with a cry:
“Bring out your dead.”
Mass burial pits opened on the city’s outskirts. Physicians wore protective clothing, including long coats and gloves, though the famous beaked mask became more common in continental Europe than England.
Daily life changed dramatically:
- Theaters closed.
- Courts suspended sessions.
- Parliament temporarily left the city.
- Commerce nearly stopped.
Food shortages emerged because farmers refused to enter London markets.
Psychological Impact
Fear played a central role in London’s 1665 Plague. People avoided neighbors and even family members. Some parents abandoned sick children; others refused medical care to escape quarantine.
Clergy wrote sermons interpreting the epidemic as moral punishment. At the same time, physicians attempted rational explanations, marking an early conflict between religious and scientific interpretations of disease.
Historians say the Bills of Mortality offered reassurance amid uncertainty. Numbers replaced rumor.
A Precursor to Modern Disease Tracking
Modern public health relies on data collection: case counts, hospital admissions, and mortality statistics. Agencies use these to recommend travel restrictions, vaccinations, or quarantine measures.
London’s 1665 Plague created a basic version of the same system.
The principles matched modern surveillance:
- identify clusters
- track spread
- inform the public
Today’s pandemic dashboards, including those used during COVID-19, operate on similar foundations.
Social Inequality and Economic Consequences
Information did not protect everyone equally.
Those with wealth escaped early and survived at higher rates. Servants, laborers, and apprentices remained in dangerous districts.
Businesses collapsed. Shipping slowed along the River Thames. International trade partners restricted contact with English vessels.
Insurance practices also changed. Merchants began calculating financial risk using mortality patterns — an early step toward modern actuarial science.
The End of the Epidemic
The outbreak peaked in September 1665. As winter approached, flea populations declined and transmission slowed.
By early 1666, deaths dropped sharply. The city gradually repopulated. Markets reopened, and government returned.
The following year, the Great Fire of London (1666) destroyed much of the medieval city. Some historians believe rebuilding with wider streets and improved sanitation reduced future outbreaks.
Long-Term Impact on Public Health
London’s 1665 Plague left a lasting institutional legacy.
Authorities continued collecting death data. Eventually Britain established civil registration systems, which recorded births and deaths nationwide.
These records enabled:
- life insurance
- urban sanitation reforms
- hospital planning
- vaccination programs
Modern epidemiology still depends on mortality statistics. Health agencies worldwide track deaths to detect emerging diseases, evaluate policy responses, and guide medical research.
FAQs About London’s 1665 Plague
What caused London’s 1665 Plague?
A bacterium (Yersinia pestis) spread by fleas living on rats.
Were the Bills of Mortality accurate?
Causes of death were estimated, but burial counts reliably showed rising mortality.
Why are they important today?
They helped create demographic statistics and disease surveillance systems still used in modern public health.